9 results
Treatment effectiveness of antibiotic therapy in Veterans with multidrug-resistant Acinetobacter spp. bacteremia
- Amanda Vivo, Margaret A. Fitzpatrick, Katie J. Suda, Geneva M. Wilson, Makoto M. Jones, Martin E. Evans, Charlesnika T. Evans
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 12 December 2023, e230
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
To describe antimicrobial therapy used for multidrug-resistant (MDR) Acinetobacter spp. bacteremia in Veterans and impacts on mortality.
Methods:This was a retrospective cohort study of hospitalized Veterans Affairs patients from 2012 to 2018 with a positive MDR Acinetobacter spp. blood culture who received antimicrobial treatment 2 days prior to through 5 days after the culture date. Only the first culture per patient was used. The association between treatment and patient characteristics was assessed using bivariate analyses. Multivariable logistic regression models examined the relationship between antibiotic regimen and in-hospital, 30-day, and 1-year mortality. Generalized linear models were used to assess cost outcomes.
Results:MDR Acinetobacter spp. was identified in 184 patients. Most cultures identified were Acinetobacter baumannii (90%), 3% were Acinetobacter lwoffii, and 7% were other Acinetobacter species. Penicillins—β-lactamase inhibitor combinations (51.1%) and carbapenems (51.6%)—were the most prescribed antibiotics. In unadjusted analysis, extended spectrum cephalosporins and penicillins—β-lactamase inhibitor combinations—were associated with a decreased odds of 30-day mortality but were insignificant after adjustment (adjusted odds ratio (aOR) = 0.47, 95% CI, 0.21–1.05, aOR = 0.75, 95% CI, 0.37–1.53). There was no association between combination therapy vs monotherapy and 30-day mortality (aOR = 1.55, 95% CI, 0.72–3.32).
Conclusion:In hospitalized Veterans with MDR Acinetobacter spp., none of the treatments were shown to be associated with in-hospital, 30-day, and 1-year mortality. Combination therapy was not associated with decreased mortality for MDR Acinetobacter spp. bacteremia.
Variations in implementation of antimicrobial stewardship via telehealth at select Veterans Affairs medical centers
- Geneva Wilson, Amanda Vivo, Daniel Livorsi, Rabeeya Sabzwari, Christopher Crnich, Robin Jump, Charlesnika Evans
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, p. s38
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Antimicrobial stewardship programs (ASPs) seek to reduce the prevalence of antimicrobial-resistant and healthcare-associated infections. There are limited infectious disease (ID) physicians and pharmacists to support these ASPs, particularly in rural areas. The Veterans Health Administration has a robust telehealth program in place. Our previous work has demonstrated the feasibility of using telehealth modalities to support ASPs at rural Veterans Affairs medical centers (VAMCs) by pairing them with an ID expert from a larger, geographically distant, VAMC. This program, dubbed the Videoconference Antimicrobial Stewardship Team (VAST), emphasizes discussion of patients undergoing treatment for an active infection and additional relevant clinical topics with a multidisciplinary team at the rural VA. VAST implementation is ongoing at VAMCs. To understand and compare the qualitative differences in implementation, we used process maps to describe the VAST at 3 VAMC dyads. Methods: Team members from each dyad participated in interviews at 3, 6, and 9 months after beginning their VAST sessions. Questions addressed several aspects of VAST implementation and included identifying cases and topics to discuss; advance preparation for meetings; the frequency and general structure of VAST meetings; and documentation including workload capture. The research team used the responses to develop process maps to permit visual display and comparison of VAST implementation. Results: The first dyad began in January 2022 and the third in March 2022. The sessions had 3 phases: preparation, team meeting, and documentation of experts’ recommendations. Tasks were shared between VAST champions at the rural VAMC and the ID experts (Fig. 1). The preparation phase showed the most variation among the 3 dyads. In general, champions at the rural VA identified cases and topics for discussion that were sent to the ID expert for review. The approaches used to find cases and the type of preparatory work by the ID expert differed. Team meetings differed in both frequency and participation by professionals from the rural site. Documentation of expert recommendations processes appeared similar among the dyads. Discussion: Each of the 3 dyads implemented VAST differently. These results suggest that the overall structure of the VAST is readily adaptable and that each site tailored VAST to suit the clinical needs, workflow, and culture of their partner facility. Future work will seek to determine which aspects in the preparation, team meeting, or documentation phases are associated with successful ASPs, including assessment of quantitative and qualitative outcomes.
Disclosures: None
Using telehealth to support antimicrobial stewardship at four rural VA medical centers: Interim analysis
- Alexandria Nguyen, Mayyadah Alabdely, Taissa Bej, Tola Ewers, Tammy Walkner Amanda Vivo, Christopher Crnich, Daniel Livorsi, Rabeeya Sabzwari, Geneva Wilson, Brigid Wilson, Corinne Kowal, Oteshia Hicks, Charlesnika Evans, Robin Jump
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, p. s110
-
- Article
-
- You have access Access
- Open access
- Export citation
-
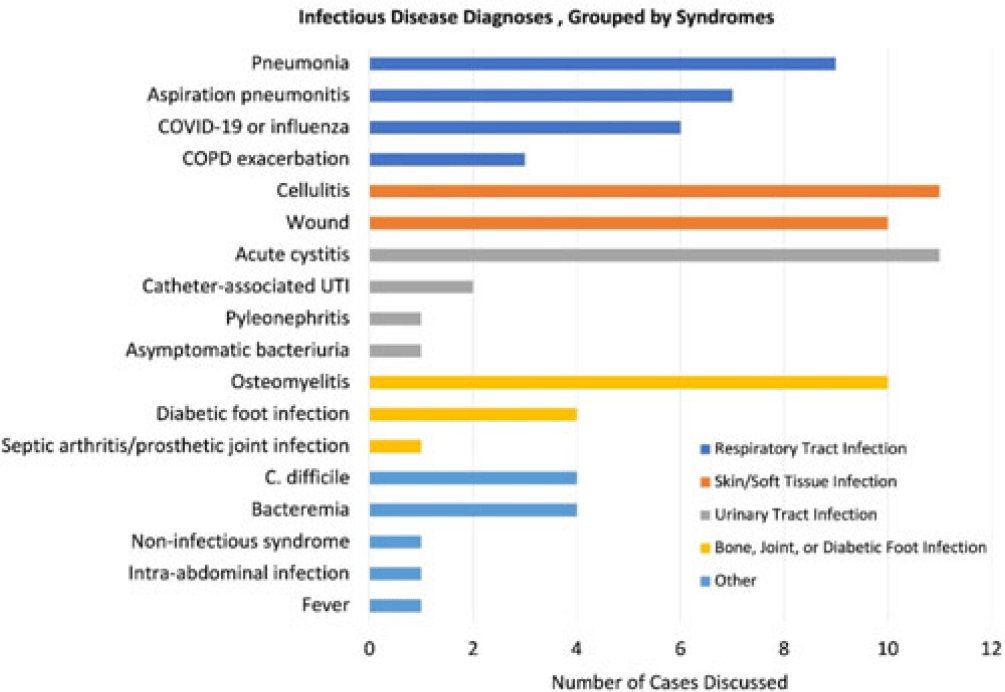
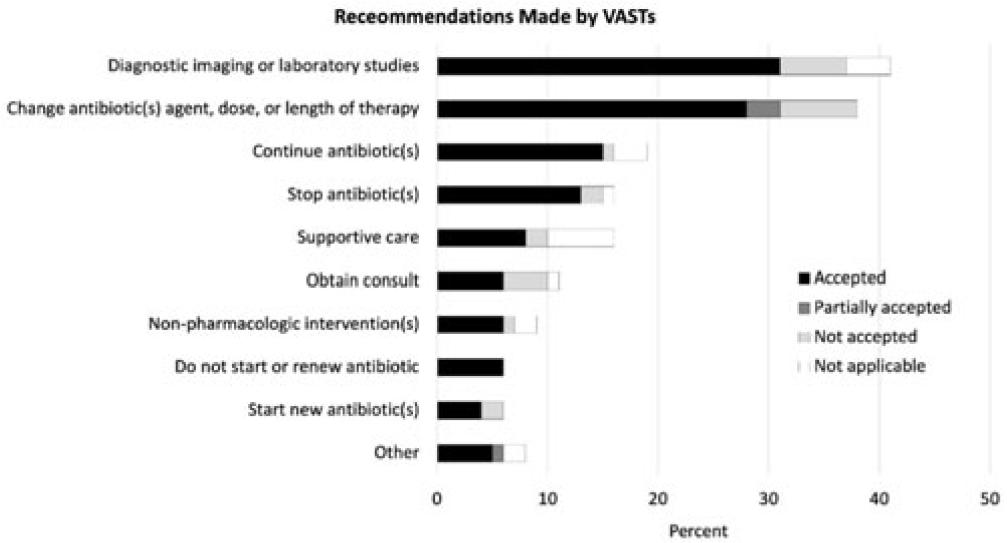
Background: Healthcare settings without access to infectious diseases experts may struggle to implement effective antibiotic stewardship programs. We previously described a successful pilot project using the Veterans Affairs (VA) telehealth system to form a Videoconference Antimicrobial Stewardship Team (VAST) that connected multidisciplinary teams from rural VA medical centers (VAMCs) with infectious diseases experts at geographically distant locations. VASTs discussed patients from the rural VAMC, with the overarching goal of supporting antibiotic stewardship. This project is currently ongoing. Here, we describe preliminary outcomes describing the cases discussed, recommendations made, and acceptance of those recommendations among 4 VASTs. Methods: Cases discussed at any of the 4 participating intervention sites were independently reviewed by study staff, noting the infectious disease diagnoses, recommendations made by infectious diseases experts and, when applicable, acceptance of those recommendations at the rural VAMC within 1 week. Discrepancies between independent reviewers were discussed and, when consensus could not be reached, discrepancies were discussed with an infectious diseases clinician. Results: The VASTs serving 4 different rural VAMCs discussed 96 cases involving 92 patients. Overall, infection of the respiratory tract was the most common syndrome discussed by VASTs (Fig. 1). The most common specific diagnoses among discussed cases were cellulitis (n = 11), acute cystitis (n = 11), wounds (n = 11), and osteomyelitis (n = 10). Of 172 recommendations, 41 (24%) related to diagnostic imaging or laboratory results and 38 (22%) were to change the antibiotic agent, dose, or duration (Fig. 2). Of the 151 recommendations that could be assessed via chart review, 122 (81%) were accepted within 1 week. Conclusions: These findings indicate successful implementation of telehealth to connect clinicians at rural VAMCs with an offsite infectious diseases expert. The cases represented an array of common infectious syndromes. The most frequent recommendations pertained to getting additional diagnostic information and to adjusting, but not stopping, antibiotic therapy. These results suggest that many of the cases discussed warrant antibiotics and that VASTs may use the results of diagnostic studies to tailor that therapy. The high rate of acceptance suggests that the VASTs are affecting patient care. Future work will describe VAST implementation at 4 additional VAMCs, and we will assess whether using telehealth to disseminate infectious diseases expertise to rural VAMCs supports changes in antibiotic use that align with principles of antimicrobial stewardship.
Disclosures: None
A qualitative approach to examining antimicrobial prescribing in the outpatient dental setting
- Ashley M. Hughes, Charlesnika T. Evans, Margaret A. Fitzpatrick, Ibuola O. Kale, Amanda Vivo, Taylor L. Boyer, Pooja A. Solanki, Gretchen Gibson, M. Marianne Jurasic, Lisa K. Sharp, Kelly L. Echevarria, Katie J. Suda
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue 1 / 2022
- Published online by Cambridge University Press:
- 24 June 2022, e102
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
To understand barriers and facilitators to evidence-based prescribing of antibiotics in the outpatient dental setting.
Design:Semistructured interviews.
Setting:Outpatient dental setting.
Participants:Dentists from 40 Veterans’ Health Administration (VA) facilities across the United States.
Methods:Dentists were identified based on their prescribing patterns and were recruited to participate in a semistructured interview on perceptions toward prescribing. All interviews were recorded, transcribed, and double-coded for analysis, with high reliability between coders. We identified general trends using the theoretical domains framework and mapped overarching themes onto the behavior change wheel to identify prospective interventions that improve evidence-based prescribing.
Results:In total, 90 dentists participated in our study. The following barriers and facilitators to evidence-based prescribing emerged as impacts on a dentist’s decision making on prescribing an antibiotic: access to resources, social influence of peers and other care providers, clinical judgment, beliefs about consequences, local features of the clinic setting, and beliefs about capabilities.
Conclusions:Findings from this work reveal the need to increase awareness of up-to-date antibiotic prescribing behaviors in dentistry and may inform the best antimicrobial stewardship interventions to support dentists’ ongoing professional development and improve evidence-based prescribing.
Opportunities for penicillin allergy evaluation in dental clinics
- Amanda Vivo, Michael J. Durkin, Ibuola Kale, Taylor Boyer, Margaret A. Fitzpatrick, Charlesnika T. Evans, M. Marianne Jurasic, Gretchen Gibson, Katie J. Suda
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue 1 / 2022
- Published online by Cambridge University Press:
- 11 April 2022, e58
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
To evaluate opportunities for assessing penicillin allergies among patients presenting to dental clinics.
Design:Retrospective cross-sectional study.
Setting:VA dental clinics.
Patients:Adult patients with a documented penicillin allergy who received an antibiotic from a dentist between January 1, 2015, and December 31, 2018, were included.
Methods:Chart reviews were completed on random samples of 100 patients who received a noncephalosporin antibiotic and 200 patients who received a cephalosporin. Each allergy was categorized by severity. These categories were used to determine patient eligibility for 3 testing groups based on peer-reviewed algorithms: (1) no testing, (2) skin testing, and (3) oral test-dose challenge. Descriptive and bivariate statistics were used to compare facility and patient demographics first between true penicillin allergy, pseudo penicillin allergy, and missing allergy documentation, and between those who received a cephalosporin and those who did not at the dental visit.
Results:Overall, 19% lacked documentation of the nature of allergic reaction, 53% were eligible for skin testing, 27% were eligible for an oral test-dose challenge, and 1% were contraindicated from testing. Male patients and African American patients were less likely to receive a cephalosporin.
Conclusions:Most penicillin-allergic patients in the VA receiving an antibiotic from a dentist are eligible for penicillin skin testing or an oral penicillin challenge. Further research is needed to understand the role of dentists and dental clinics in assessing penicillin allergies.
Management of Pseudomonas aeruginosa Bloodstream Infection and Impact on Health Outcomes
- Swetha Ramanathan, Margaret Fitzpatrick, Fritzie Albarilo, Katie Suda, Linda Poggensee, Amanda Vivo, Martin Evans, Makoto Jones, Nasia Safdar, Geneva Wilson, Charlesnika Evans
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, p. s22
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Gram-negative bacteria cause a variety of hospital-associated infections (HAIs). Of concern is Pseudomonas aeruginosa, which is a leading cause of HAIs. Early and adequate therapy of P. aeruginosa blood stream infection (BSI) is associated with decreased mortality. Additionally, infectious disease consultation has also shown to improve health outcomes, streamline care, and decrease costs. Therefore, the goal of this study was to describe treatment of P. aeruginosa BSI and impact of infectious disease consultations on health outcomes. Methods: In this retrospective cohort study, we analyzed national VA medical, encounter, pharmacy, microbiology, and laboratory data from January 1, 2012 to December 31, 2018. The cohort included all hospitalized adult veterans (aged ≥18 years) who had a positive blood culture for P. aeruginosa. Only the first P. aeruginosa blood culture per patient was included, and duplicate cultures within 30 days were removed. Treatment was identified within −2 to +5 days of the culture date. Multidrug-resistant (MDR) cultures were identified based on resistance to at least 1 agent in at least 3 or more antimicrobial categories tested. Multivariable logistic regression models were fit to assess infectious disease consultations and adequate treatment on in-hospital mortality and 30-day mortality. Results: In total, 3,256 patients had a BSI with P. aeruginosa, of which 386 (11.5%) were MDR. Most of these patients were male (97.5%), >65 years of age (70.9%), and non-Hispanic white (63.8%). Also, 784 patients (23.3%) died during hospitalization and 870 (25.8%) died within 30 days of their culture. In multivariable regression models, infectious disease consultations were associated with decreased odds of in-hospital mortality (odds ratio [OR], 0.64; 95% confidence interval [CI], 0.53–0.77) and 30-day mortality (OR, 0.56, 95% CI, 0.48–0.67) even after adjusting for age, race, care setting, Charlson score, and prior healthcare exposures. Furthermore, inadequate definitive treatment was associated with increased odds of in-hospital mortality (OR, 2.77; 95% CI, 1.35–5.69) and 30-day mortality (OR, 2.37; 95% CI, 1.18–4.79), even after adjusting for age, Charlson score, care setting, and prior healthcare exposures. In addition, carbapenem treatment was associated with increased odds of in-hospital mortality (OR, 1.38; 95% CI, 1.12–1.70) and 30-day mortality (OR, 1.49; 95% CI, 1.22–1.81), whereas fluoroquinolone treatment was associated with lower odds of in-hospital mortality (OR, 0.49; 95% CI, 0.41–0.59) and 30-day mortality (OR, 0.60; 95% CI, 0.50–0.71). Finally, extended-spectrum cephalosporin was also associated with lower odds of in-hospital mortality (OR, 0.82; 95% CI, 0.68–0.98). Conclusions: Use of infectious disease consultations and any adequate definitive treatment for those with P. aeruginosa BSI lowered odds of in-hospital and 30-day mortality. Early consultation with infectious disease physicians regarding adequate treatment has direct positive impact on clinical outcomes for patients with P. aeruginosa BSI.
Funding: No
Disclosures: None
Treatment of Extensively Drug-Resistant (XDR) Acinetobacter in US Veterans’ Affairs (VA) Medical Centers
- Margaret Fitzpatrick, Katie Suda, Linda Poggensee, Amanda Vivo, Geneva Wilson, Makoto Jones, Martin Evans, Nasia Safdar, Charlesnika Evans
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, p. s71
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Infections caused by Acinetobacter spp are often healthcare acquired and associated with high mortality. Extensively drug-resistant (XDR) Acinetobacter are nonsusceptible to at least 1 agent in all but 2 or fewer antibiotic classes. Few of the new antibiotics targeting multidrug-resistant gram-negative bacteria are effective against XDR Acinetobacter. Recent national guidelines for treatment of resistant gram-negative infections do not include Acinetobacter, leaving a knowledge gap in best practices. Methods: This retrospective cohort study included microbiology, clinical, and pharmacy data from all patients hospitalized between 2012 and 2018 at any Veterans’ Affairs medical center who had cultures that grew XDR Acinetobacter spp. Bivariate unadjusted analyses compared clinical outcomes by monotherapy versus combination therapy. Using mixed-effects ordinal logistic regression, propensity score–adjusted models accounting for severity of illness and other variables associated with treatment were fit to compare outcomes. Results: Of 11,546 patients with 15,364 cultures that grew Acinetobacter spp, 408 patients (3.5%) had 666 cultures (4.3%) with XDR Acinetobacter. Moreover, 276 of these patients (67.6%) had gram-negative targeted antibiotic treatment within −2 to +5 days from the culture. Furthermore, 118 patients (42.8%) received monotherapy, most commonly piperacillin-tazobactam (n = 54, 45.7%) or an anti-Pseudomonas cephalosporin (n = 21, 17.8%). Also, 158 (57.2%) patients received combination therapy, most commonly a carbapenem (n = 93, 58.9%) and/or polymyxin (n = 68, 43.0%). Moreover, 41 patients (25.9%) received both a carbapenem and polymyxin. In both unadjusted and adjusted analyses, there were no significant differences in the odds of 30-day mortality (aOR, 1.43; 95% CI, 0.86–2.38) or 1-year mortality (aOR, 1.04; 95% CI, 0.68–1.60) between combination therapy and monotherapy groups. Among 264 patients (96%) whose cultures occurred during an inpatient or long-term care admission, unadjusted analyses showed increased odds of in-hospital mortality (OR, 1.89; 95% CI, 1.08–3.29) and longer postculture length of stay in the combination therapy group: median, 23 days (IQR, 11–57) versus 14 days (IQR, 7–32) (P = .02). However, with propensity score adjustment, these associations were no longer significant. Furthermore, there was no significant difference in odds of 90-day readmission between groups in either unadjusted or adjusted analyses (aOR, 1.20; 95% CI, 0.74–1.95). Conclusions: In this large national cohort of patients with XDR Acinetobacter cultures, more patients received combination therapy than monotherapy, and carbapenems and polymyxins were the most-used classes. However, there were no significant differences in outcomes between patients receiving combination therapy and monotherapy, suggesting lack of clinical benefit to the common practice of treating XDR Acinetobacter infections with multiple antibiotics. Further research is needed to determine optimal treatment strategies for this pathogen.
Funding: No
Disclosures: None
Epidemiology and Clinical Outcomes Associated With Extensively Drug-Resistant (XDR) Acinetobacter in US Veterans’ Affairs Health Care
- Margaret Fitzpatrick, Katie Suda, Linda Poggensee, Amanda Vivo, Marissa Gutkowski, Geneva Wilson, Charlesnika Evans
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s62-s63
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Infections caused by Acinetobacter spp are often healthcare acquired, difficult to treat, and associated with high mortality. Extensively drug-resistant (XDR) Acinetobacter are nonsusceptible to at least 1 agent in all but 2 or fewer antimicrobial classes. Epidemiologic and outcome data for XDR Acinetobacter are limited and have largely been reported outside the United States. This national cohort study describes epidemiology, clinical characteristics, and outcomes for patients with XDR Acinetobacter in VA health care. Methods: This was a retrospective cohort study including microbiology and clinical data from all patients hospitalized between 2012 and 2018 at any VA medical center who had cultures that grew XDR Acinetobacter spp. Performance and reporting of bacterial speciation and antibiotic susceptibility testing were performed by each VA laboratory according to their protocol. Descriptive statistics were used to summarize data. Results: Of 11,541 unique patients with 15,358 cultures that grew Acinetobacter spp during the study period, 410 (3.6%) patients had 670 (4.4%) cultures that grew XDR Acinetobacter. Mean age was 68 years (SD, 12.2 years) and the median Charlson comorbidity index was 3 (IQR, 1–5). The greatest proportion of isolates were from the respiratory tract (n = 235, 35%) followed by urine (n = 184, 28%). The South had the greatest proportion of patients with XDR Acinetobacter (n = 162, 40%); almost all patients were seen at urban VA medical centers (n = 406, 99%). Most patients (n = 335, 82%) had had antibiotic exposure in the prior 90 days, most commonly vancomycin (n = 238, 65%) and third- or fourth-generation cephalosporins (n = 155, 38%). Most patients (n = 334, 81%) also had a hospital or long-term care admission in the prior 90 days. Fig. 1 shows antibiotic susceptibilities of XDR Acinetobacter isolates; polymyxins, tigecycline, and minocycline demonstrated the highest susceptibility. In-hospital mortality occurred in 90 patients (22%), 30-day mortality in 97 patients (24%), and 1-year mortality in 198 patients (48%). Of 93 patients, 23% were readmitted to the hospital within 90 days. Conclusions: Providers should maintain a heightened suspicion for infection with XDR Acinetobacter spp in older patients seen at urban medical centers who have had recent healthcare and antibiotic exposures, particularly if they have respiratory or urinary tract infections. Isolation of XDR Acinetobacter is associated with high in-hospital and 30-day mortality. New antibiotics targeting MDR gram-negative bacteria generally lack activity against Acinetobacter, leaving polymyxins, tigecycline, and minocycline as the only limited treatment options. Therefore, novel antibiotics for XDR Acinetobacter are urgently needed.
Funding: None
Disclosures: None
Epidemiology and clinical outcomes associated with extensively drug-resistant (XDR) Acinetobacter in US Veterans’ Affairs (VA) medical centers
- Margaret A. Fitzpatrick, Katie J. Suda, Linda Poggensee, Amanda Vivo, Marissa Wirth, Geneva Wilson, Martin Evans, Charlesnika T. Evans
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 3 / March 2021
- Published online by Cambridge University Press:
- 30 September 2020, pp. 305-310
- Print publication:
- March 2021
-
- Article
- Export citation
-
Objective:
Although infections caused by Acinetobacter baumannii are often healthcare-acquired, difficult to treat, and associated with high mortality, epidemiologic data for this organism are limited. We describe the epidemiology, clinical characteristics, and outcomes for patients with extensively drug-resistant Acinetobacter baumannii (XDRAB).
Design:Retrospective cohort study
Setting:Department of Veterans’ Affairs Medical Centers (VAMCs)
Participants:Patients with XDRAB cultures (defined as nonsusceptible to at least 1 agent in all but 2 or fewer classes) at VAMCs between 2012 and 2018.
Methods:Microbiology and clinical data was extracted from national VA datasets. We used descriptive statistics to summarize patient characteristics and outcomes and bivariate analyses to compare outcomes by culture source.
Results:Among 11,546 patients with 15,364 A. baumannii cultures, 408 (3.5%) patients had 667 (4.3%) XDRAB cultures. Patients with XDRAB were older (mean age, 68 years; SD, 12.2) with median Charlson index 3 (interquartile range, 1–5). Respiratory specimens (n = 244, 36.6%) and urine samples (n = 187, 28%) were the most frequent sources; the greatest proportion of patients were from the South (n = 162, 39.7%). Most patients had had antibiotic exposures (n = 362, 88.7%) and hospital or long-term care admissions (n = 331, 81%) in the prior 90 days. Polymyxins, tigecycline, and minocycline demonstrated the highest susceptibility. Also, 30-day mortality (n = 96, 23.5%) and 1-year mortality (n = 199, 48.8%) were high, with significantly higher mortality in patients with blood cultures.
Conclusions:The proportion of Acinetobacter baumannii in the VA that was XDR was low, but treatment options are extremely limited and clinical outcomes were poor. Prevention of healthcare-associated XDRAB infection should remain a priority, and novel antibiotics for XDRAB treatment are urgently needed.





